This case is written by Dr. Kyla Caners. She is a staff emergency physician in Hamilton, Ontario and the Simulation Director of McMaster University’s FRCP-EM program. She is also one of the Editors-in-Chief here at EmSimCases.
Why it Matters
The majority of STEMI presentations to the ED are quite straight-forward to manage: expediency and protocolization are of the utmost importance. However, when a patient presents with cardiogenic shock as a result of their STEMI, more nuanced care is required. In particular, the patient must be stabilized in order to facilitate the definitive treatment of cardiac catheterization. This case highlights some of those nuances, including:
- The need for vasopressor support and possibly inotropic support in patients with cardiogenic shock
- The challenges associated with intubating a hypotensive and hypoxic patient
- The importance of optimizing the patient’s status as best as possible prior to intubation (whether via BiPAP, PEEP valve, push-dose pressors, or otherwise)
Clinical Vignette
A 55-year-old male presents to the ED with EMS as a STEMI activation. He arrives being bagged by EMS for hypoxia. His initial EMS call was for chest pain and he has significantly deteriorated en route. He has a history of smoking, hypertension, diabetes, and hypercholesterolemia. No prior cardiac history.
Case Summary
A 55-year-old man presents to the ED as a STEMI call. He is profoundly hypotensive with low O2 sats and obvious CHF. The patient’s blood pressure will transiently respond to fluid resuscitation. The ECG will show anterolateral ST elevation. The team will need to prepare for intubation while activating the cath lab. They will also need to start vasopressors. The patient will remain hypotensive until an inotrope like dobutamine is initiated. If unsafe medications are chosen for intubation, the patient will have a VT arrest.
Download the case here: STEMI with Cardiogenic Shock
ECG for the case found here:
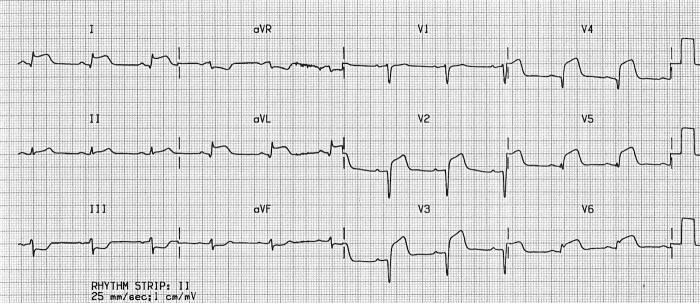
(ECG source: https://lifeinthefastlane.com/ecg-library/lateral-stemi/)
Pre-intubation CXR for the case found here:
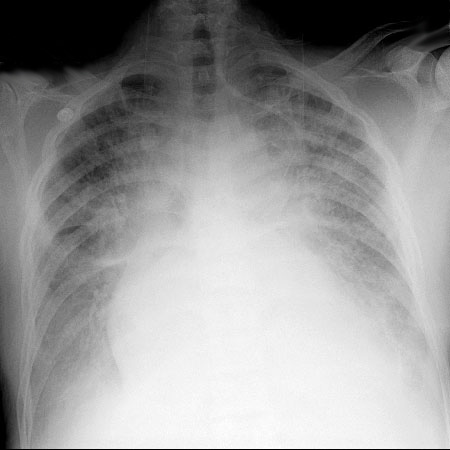
(CXR source: https://www.med-ed.virginia.edu/courses/rad/cxr/pathology2Bchest.html)
Post-intubation CXR for the case found here:
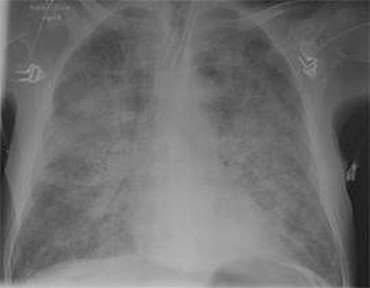
(CXR source: https://heart-conditions.knoji.com/learning-about-and-coping-with-congestive-heart-failure/)