This case was written by Dr. Stephen Watson with support from Drs. Lee Graham and Jared Baylis.
Dr. Stephen Watson (@spraytansteve) is a PGY-2 Emergency Medicine resident at the University of British Columbia. His interests include trauma medicine and medical education. He is engaged in research exploring novel regional anesthesia techniques in trauma. He completed his B.Sc. in Microbiology at UBC-Okanagan and went on receive his MD from UBC’s Southern Medical Program.
Dr. Lee Graham (@leegarthgraham) is an emergency physician and medical educator at Kelowna General Hospital. He completed his FRCPC in Emergency Medicine in Calgary and his Masters of Tropical Medicine and International Health at the London School of Hygiene and Tropical Medicine. He has an in interest in medical education, global health, and quality improvement. He has taught and spoken locally, and internationally on these topics. He is a member of the UBC and Kelowna Emergency Medicine Residency Training Committee.
Dr. Jared Baylis (@baylis_jared) is an emergency physician and simulation educator at Kelowna General Hospital. He is also the Medical Director of Simulation for the Interior Health Authority as well as the Medical Education Sim Lead for UBC’s Southern Medical Program. He has an interest in simulation, medical education, and administration/leadership and completed his simulation fellowship through the Centre of Excellence for Simulation Education and Innovation in Vancouver, BC, his residency at UBC (@KelownaEM), and medical school at Queen’s University. Jared is currently a MMEd student through Dundee University.
WHY IT MATTERS
Orbital compartment syndrome (OCS) is a vision threatening emergency that requires decisive and timely action in the form of lateral canthotomy and cantholysis.
Today’s case provides a description of a porcine task training model for lateral canthotomy and includes a simple simulation case to go along with it. This model was recently used for the @KelownaEM annual resident procedure day.
Background
OCS is a rarely encountered clinical entity that arises after orbital trauma or as a complication of oculofacial surgery1. Its presence is suggested based on history and clinical examination which are often remarkable for recent orbital trauma or manipulation accompanied by decreased visual acuity, afferent pupillary defect, proptosis, and increased intra-ocular pressure 2. The bony architecture of the orbit creates an enclosed space in which increased pressure can rapidly begin to compress vital structures such as the optic nerve, which can lead to irreversible vision loss in the affected eye.
Once the diagnosis of OCS is made, the decision to carry out a lateral canthotomy (LC) must be made expeditiously as permanent vision loss can occur within 90-120 minutes from symptom onset3. Though the LC is a simple and potentially vision saving procedure that is in the scope of practice of emergency medicine physicians, many will have had minimal experience carrying out the procedure in clinical practice. Numerous models have been developed to train physicians in the proper technique of LC; cadaveric models provide some of the highest fidelity models available for LC but their use is limited by cadaver availability and embalmed cadaver’s globes often lose their volume, making the model low fidelity4,5. Synthetic anatomical models are more readily available, but their cost and fidelity can vary substantially. Animal models provide a happy medium in terms of cost and fidelity. Recently the UBC EM Interior residency cohort trialed the use of porcine facial models as task trainers for simulated LCs.
CASE SUMMARY
A 25 y/o M pitching in a Sunday baseball game is hit in the face by a line drive. He is brought to the ED by his friends complaining of decreased visual acuity to his right eye accompanied by significant right peri-orbital swelling. At triage his VA is OD 20/100 OS 20/25 but at the time of assessment VA OD is limited to detection of light and his pupil is fixed and dilated, extra-ocular movements are intact. The team should recognize the need for lateral canthotomy based on the history and physical exam findings (including IOP) and mobilize the appropriate resources for bed-side lateral canthotomy as well as the need for emergent ophthalmology consult.
Materials and Methods
Prior to carrying out the procedure in the simulation lab, learners were provided with educational resources outlining the indications for and methods of carrying out the LC.
Recently butchered porcine heads were procured from a local processor. Each model allowed for two LC procedures to be carried out allowing for one learner to carry out bilateral LCs or for two learners to practice on the same model. To mimic the clinical findings of proptosis, chemosis, and increased intra-ocular pressure seen with retrobulbar hematoma/orbital compartment syndrome, 20mL of normal saline was instilled retro-orbitally with a 22G 1.5-inch needle via a medial approach.
For the procedure itself each learner was provided with alcohol swabs for skin sterilization, a 10mL syringe with 27G needle for instillation of local anesthetic, a mosquito hemostat for crush hemostasis, forceps for tissue manipulation, and iris scissors for tissue dissection and cantholysis.
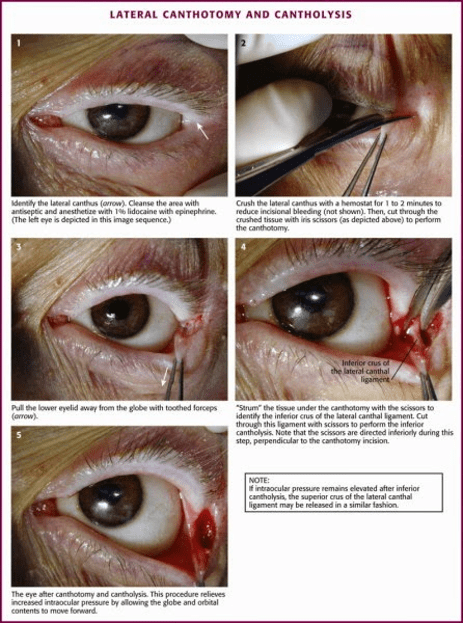
Once the skin overlying the lateral orbit was cleaned a small volume of local anesthetic was instilled, after which the hemostat was applied to the lateral canthus for 30-60 seconds to achieve hemostasis. After sufficient time had elapsed the hemostat was released, and the iris scissors were used to cut along the path of compression through all layers of tissue down to the level of bone with care being taken to direct instruments laterally, toward the orbital rim and away from the globe to minimize the risk of iatrogenic globe injury. Forceps were then used to retract the lower eyelid and expose the inferior crus of the lateral canthal tendon at its position just inferior and posterior to the lateral canthal fold. The location of the tendon can be confirmed by palpation, with its characteristic band-like texture belying its location. Once located, the tendon was cut with the iris scissors to decompress the orbital compartment, again taking care to avoid injury to the globe. The superior crus can be similarly located via palpation and cut should the orbital compartment require additional decompression. 6,7
Discussion
Porcine facial models provided an excellent task trainer for LC in the simulation lab. Their orbital anatomy closely approximates that of humans and the instillation of 20mL saline into the retro-orbital space mimics the clinical presentation of OCS quite well. There are some limitations when it comes to the use of porcine facial models. The skin of the porcine model is significantly thicker than human skin and requires more force to dissect. Additionally, there are some fidelity shortcomings with the porcine model, the lack of pupillary reactivity makes it difficult to evaluate successful decompression and without active bleeding the LC site is much cleaner in the porcine model than can be expected in vivo. Despite these minor issues the porcine facial models proved to be outstanding task trainers.
DOWNLOAD THE CASE HERE:
References
- Gordon, S., & Macrae, H. (1950). Monocular Blindness As A Complication Of The Treatment Of A Malar Fracture. Plastic and Reconstructive Surgery, 6(3), 228-232. doi:10.1097/00006534-195009000-00005
- Bailey, W. K., Kuo, P. C., & Evans, L. S. (1993). Diagnosis and treatment of retrobulbar hemorrhage. Journal of Oral and Maxillofacial Surgery, 51(7), 780-782. doi:10.1016/s0278-2391(10)80422-7
- Popat, H., Doyle, P., & Davies, S. (2007). Blindness following retrobulbar haemorrhage—It can be prevented. British Journal of Oral and Maxillofacial Surgery, 45(2), 163-164. doi:10.1016/j.bjoms.2005.06.028
- Credland, T. (2015). 0173 The development of a model to simulate an intra ocular bleed and lateral canthotomy. Technical Innovations/tech Room Topics. doi:10.1136/bmjstel-2015-000075.15
- Patel, S. R., Mishall, P., & Barmettler, A. (2019). A human cadaveric model for effective instruction of lateral canthotomy and cantholysis. Orbit, 39(2), 87-92. doi:10.1080/01676830.2019.1600151
- Rowh, A. D., Ufberg, J. W., Chan, T. C., & Vilke, G. M. (2015). Lateral Canthotomy and Cantholysis: Emergency Management of Orbital Compartment Syndrome. The Journal of Emergency Medicine, 48(3), 325–330.
- Mahon, B. M., & Desai, B. K. (2016). Lateral Canthotomy. Atlas of Emergency Medicine Procedures, 305-308. doi:10.1007/978-1-4939-2507-0_52