**July 28, 2025 – Scroll to the bottom for new rapid cycle case content**
This primer on Rapid Cycle Deliberate Practice was written by academic pediatric emergency medicine specialist and simulation guru Dr. Quang Ngo. He is a staff physian at McMaster Children’s Hospital, scholar with the McMaster Education Research, Innovation and Theory (MERIT) program and Founding Program Director for the Pediatric Emergency Medicine subspecialty residency program.
The Problem
Sam is on faculty at an academic pediatric residency program with an interest in simulation enhanced education. Sam’s interest in simulation started in fellowship and she’s since taken multiple debriefing courses and regularly attended medical simulation conferences since joining the faculty in an effort to expand her community of practice. She’s also a keen and recognized medical educator within the department. After the program identified a gap in resuscitation training opportunities for their learners, she set up a longitudinal simulation based training curriculum for the learners of the curriculum, based on the objectives of training of the specialty and a needs assessment conducted by the program of relevant stakeholders.
The program has been active for 2 years and Sam has been reviewing the program evaluation data for the simulation curriculum. While the overall feedback has been positive, there are some areas of weakness that have been brought up consistently. Feedback from the junior learners has included comments about how they can feel very lost and confused when they first join the simulation training sessions because of the chaos they feel in the room; they feel that it’s difficult to learn how to incorporate the basics of CPR and advanced airway management into a more complex scenario. The senior learners appreciate the opportunities but find it can be frustrating after debriefing to not be able to practice what they identified were gaps in their performance, especially given that the size of the program was large and they may only get 4 or 5 sessions per year.
Given the above, Sam is concerned that her learners aren’t maximizing the effectiveness of their learning and sets about looking for a solution the problem presented by her learners.
Nothing is as practical as a good theory – Deliberate Practice
Attributed to Dr. K. Anders Ericsson and his extensive study of expertise, deliberate practice is the idea that expert level performance is not the result of innate talents, but rather acquired through years of focused practice in a specific area. Moreover, not all practice is equal and that it is deliberate practice which distinguishes people who attain a basic proficiency and someone who becomes a master in that area.
Studying fields as diverse as music, sports and chess, Ericsson found that innate abilities had little to do with the development of expertise. Rather, years of practice appeared to determine ability rather than genetic predispositions (with the exception of height and body size – height is essential to play elite level basketball, and cannot be modified regardless of practice). Even amongst those considered gifted or talented from an early age, years of practice appears to predict their ability to acquire expert levels of ability.
Core to the theory is the idea that not all practice is equal – simply practicing something repetitively does not develop the skills necessary for mastery (ie. having experience does not make you an expert – driving for 10 years does not make you an excellent driver). Deliberate practice appears to have the following characteristics in common, regardless of the field studied:
- Requires a motivated learner
- Requires a specific and attainable goal with a well defined task
- Requires immediate feedback, usually with the help of an instructor or coach
- Requires time to practice with incorporation of the feedback
Many have described deliberate practice feeling uncomfortable, as the task and goal are often just beyond the current skillset of the learner and requires focus and effort.
Rapid Cycle Deliberate Practice vs Traditional Sim Teaching
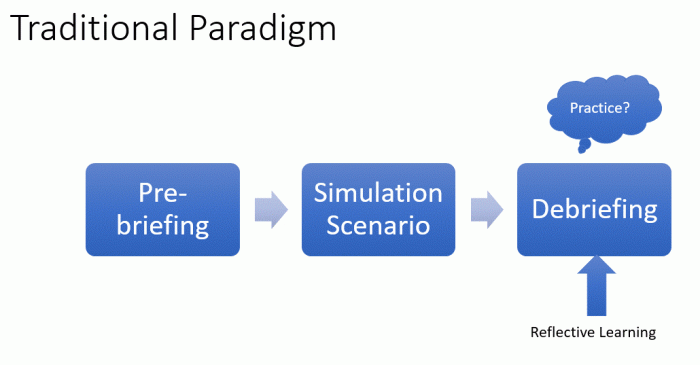
Traditional medical simulation follows a reflective learning model: following a prebrief, the learners would go through a full simulation session and then undergo a facilitated debrief with the learners reflecting on their performance and exploring the cognitive frames behind their actions.
Rapid Cycle Deliberate Practice (RCDP) uses the theory of deliberate practice to create an environment in which skills building is accomplished through short cycles of simulation interrupted by micro-debriefing and followed by re-engagement in the simulation in order to “overlearn” (practicing/drilling a newly acquired skill beyond the point of initial mastery). This isn’t to say that there is no place for reflective practice after debriefing, but rather that there may be situations in which opportunities to practice with interruptions in the traditional debriefing methods may be desirable.
RCDP was developed and described by Dr. Hunt and colleagues as a response to a program of research looking at delays and errors in CPR in pediatrics residents. In one of their studies looking at the above, they found that the majority of their learners did not meet the standard of initiating CPR and defibrillating a simulation patient in a prespecified amount of time, regardless of training level or enrolment in courses. Most interestingly (and perhaps obviously in retrospect), they found the main predictor of a learner defibrillating a simulated patient effectively was if they had actually done it previously. As you imagine, for certain competencies, mastery is of utmost importance and that learning something efficiently matters given the amount of time with a learner or team may be limited.
Hunt and colleagues describe RCDP as “rapid cycle between deliberate practice and directed feedback until skill mastery is achieved” after which progression in case difficulty can proceed. This model includes drilling/practicing the “right way” to take advantage of overlearning as described above); relying on expert feedback to show the learner the gold standard rather than having them figure it out; and psychological safety.
In considering whether or not to use RCDP as a simulation method, it is important to understand in what contexts it is most likely to be successful. Consider:
- When teaching them “how” is as important as teaching them “what”
- When repetition and muscle memory are important (ie. CPR)
- When pattern recognition is important – consider if/and protocols such as if you see ventricular fibrillation, you should defibrillate
- When communication scripts are important
- When choreography is important – consider the organization of a chaotic room in the first five minutes of a resuscitation
- When practicing the use of cognitive aids – consider a Broselow tape or a ACLS card and knowing where the necessary information is located
Live. Die. Repeat. The Mechanics of RCDP
Taking time at this point to orient the learner is important to establish the expectations of the session, teach them the process and how it differs from traditional simulation and to create an atmosphere of psychological safety where the learner understands that you are trying to help them perform at their best.
- “Vegas” Rules – emphasize confidentiality and that what happens in the session stays in the session
- Prepare them for focussed feedback – learners are not used to being interrupted and this can be very disorientating so making sure they understand this will happen is important
- Normalizing mistakes – make clear that we are looking to help you succeed and make clear the goals of the session
- Creating an encouraging environment – being a coach means being interested, invested in their progress and enthusiastic
- Initial simulation to identify gaps and confirm need for training – don’t interrupt the first attempt – this serves 2 purposes: first, it leverages principles of adult learning theory and shows them that they themselves have a gap; secondly, it allows you as an instructor to diagnose the learner
- Level up – start with easy cases with things seen and skills needed most frequently thus getting most repetition – build up to required skills that are essential but used less frequently
- Drill – interrupt when they make a mistake on a skill previously worked on – don’t let them move on until the skill/idea is incorporated.
- Back up plan – plan for additional lessons/skills if the team is advancing faster than expected or be prepared to focus on essential skills if time is running out
Remember that if something is not working despite multiple attempts at fixing the problem with a focused debriefing approach, it may be necessary to go back to your advocacy/inquiry model in order to try and understand the reason why something isn’t working.
Back to the Problem…
Sam identifies Rapid Cycle Deliberate Practice (RCDP) as a potential solution to her simulation program dilemma. She decides to separate the 1st year residents from the rest of the residents and develops a RCDP curriculum for them specifically aimed at developing the skills of managing the “First Five Minutes” of a resuscitation. These objectives include mastery of basic skills such as Bag-Valve-Mask Ventilation, high quality CPR, Defibrillation, Intraosseous Placement, organization of a team during a resuscitation and effective leadership/followership. The plan is to master these skills over the course of the first 6 – 12 months of their first year of residency before joining the upper year residents. She also plans a refresher RCDP session yearly for upper year residents in order to reinforce their learning of the basics of setting up a resuscitation and their knowledge of PALS algorithms. She reasons that if they spent their first year mastering these foundational skills, they could space out the sessions in later years knowing that they will need less frequent refreshers over time.
**New** RCDP Cases
July 28, 2025 – Check out these three cases designed for rapid cycle deliberate practice. There is an adult one, a pediatric one, and a neonatal one for you to use to seek resuscitation mastery. JoAnne Slinn (Simulation Knowledge Coordinator at the Pritchard Simulation Center – https://bcsimulation.ca/sim-programs/ih-sim/programs/psc/) has done a masterful job of putting these cases together and has tested them thoroughly with several groups of learners. Let us know what you think!
Some Suggested Sim Cases
References
Education Theory Made Practical Volume 2. 2018. Academic Life in Emergency Medicine.
Ericsson KA. 1993. The role of deliberate practice in the acquisition of expert performance psychological review. Psychological Review 100(3):363-406. DOI:10.1037//0033-295X.100.3.363.
Hunt et al. 2014. Pediatric resident resuscitation skills improve after RCDP training. Resuscitation Jul;85(7):945-51. doi: 10.1016/j.resuscitation.2014.02.025.
